So your skin is covered in itchy red welts, and you’re desperate for just about anything that will make it go away. When those welts start to pop up on your skin, you’re going to want to know how to get rid of hives from the comfort of your home—and how to do it fast! So let’s dive into the best hives treatment options that you can do at home. But first, make sure it’s not something more serious.
What are hives?
Before determining how to get rid of hives, it’s important to understand what they are. Hives are often an irritating side effect of allergies. Although the name sounds like a place where bees live, hives can happen when you encounter just about anything you’re allergic to, not just stinging pests.
They can happen anywhere on the body, but usually they are triggered by something. Different types of hives respond best to different kinds of treatment. Before you do anything to treat your hives, you need to know what you’re actually dealing with.
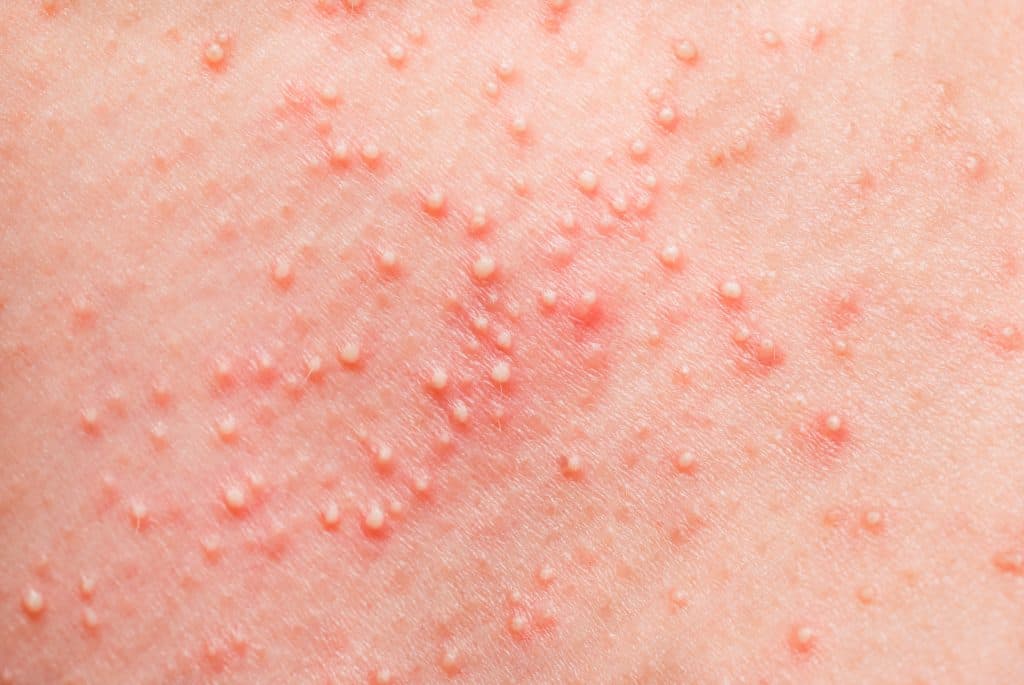
Are there red blotches that look like welts on your skin? Is it itchy? Try pressing on it. Does it blanch, or turn white when you press down, and then turn pink or red again when you let go? If the answer to all three questions is yes, you’ve probably got urticaria, the medical term doctors use for hives.
Unlike rashes, which tend to spread and don’t blanch when touched, hives tend to stick to one part of the body and blanch, says allergist Tania Elliott, MD, a spokesperson for the American College of Allergy, Asthma, and Immunology and chief medical officer at EHE. They can show up anywhere on the body, and the itch can be mild to severe, making you want to tear at your skin with sandpaper for some relief.
How to Get Rid of Hives
Now for the good news: Most people’s hives are acute, meaning they will go away within 24 hours. Fortunately, treating acute urticaria (hives) at home is fairly simple. This is how to get rid of hives at home.
Cold Compress
If you want to go the natural route, hit your kitchen. Grab a plastic baggie and fill it with ice cubes. Wrap the ice in a thin towel and place it up against the hives.
Your body’s nerves will only be able to send one response to the brain, Elliott says, so your body will either process the cold or the itch. The cold from the ice will overwhelm and quell the itch, at least temporarily. It’s not a hives treatment, per-say, but it will help with the annoying side effect, itchiness.

Antihistamine
One of the most common and effective hives treatment options is an antihistamine. Elliott suggests hitting the pharmacy for a non-sedating or non-drowsy one. Brand name products like Claritin and Zyrtec or generic versions will all do the trick, taking the itch out of hives in about 20 minutes.
Doctors often turn to prescription-strength antihistamines to keep the redness and itchiness at bay. Medications such as Allegra or Zyrtec, which are available over the counter to be taken daily, are often increased to twice-a-day prescriptions to help get rid of hives.
There are some natural antihistamine options as well, like vitamin C and quercetin, which is found in apples and onions.
Aloe Vera
Another method for how to get rid of hives is to apply some aloe vera to the affected area, according to esthetician Ildi Pekar.
Not only is the aloe plant known for its skin-healing properties, it’s also naturally cooling, so it offers a similar sensation to ice without the need to hold a baggie full of ice cubes against your skin.

Prednisone
Prednisone, a steroid, can keep hives at bay, Gandhi says, but it has drawbacks: Once you stop prednisone, the hives tend to come back.
“Prednisone on a long-term basis also has a lot of side effects, so it’s not a real solution in terms of solving hives on a long-term basis,” he adds.
Zantac
Another hives treatment option is Zantac, an over-the-counter medication. It’s best known for treating acid reflux or heartburn, may also be added on for hives sufferers, as it’s been found to be effective for soothing urticaria.
Xolair
If the hives don’t respond to the pill options, the next step is an injectable medication called Xolair, Gandhi says, which you receive at your allergist’s office. If you’ve heard your friends talking about their allergy shots, this is one of them.
Because you have to return to the doctor’s office monthly, it can be inconvenient for patients, and it’s typically expensive, requiring prior authorization from insurance companies.
“It has its own set of side effects that one has to keep in mind,” Gandhi warns, “But it works pretty good for the hives which are not responding to any of the other [medications].”
How to Get Rid of Hives That Are Recurring
Regardless of treatment, and regardless of the cause, doctors hope that the hives will eventually go away, and for most people they do, Elliott says. About half of chronic hives sufferers will see them simply disappear within a year. Others may see them go sometime within two years.
If they don’t disappear, and no other symptoms crop up that cause doctors to investigate further, a daily antihistamine regimen becomes a part of life. Even there, the news isn’t all bad.
Hilary H. has managed to get her hives under control with twice-daily Allegra, and she can go weeks without a hive popping up. Then again, it’s not all smooth sailing. “Then suddenly something will set them off without warning, and I’ll add another antihistamine (Zyrtec or Pepcid),” she says. “Typically that gets them back under control within a day or so.”
“Usually any individual hive or patch of hives doesn’t last for more than 24 hours, although more might crop up that will also last 24 hours,” she adds. “ If they’re really itching or painful, I find that cooling my skin can provide quick temporary relief. So I might run my hands under cold water or take a cool shower or hold an ice pack on them to take the edge off. That really helps!”

What Not to Do to Treat Hives
One important thing not to do when determining how to get rid of hives? Don’t scratch furiously at your skin, no matter how much you are tempted. Deep scratching opens up the skin, which can lead to infection, taking a simple case of “treatable at home” hives into “it’s time to see the doctor now” territory.
Of course, if the hives aren’t your only symptom and you’ve got a fever and chills along with those red welts, don’t stick around the house. Call your doctor immediately. It may be nothing more than a simple virus that you’ll kick in 24 hours, but it’s better to be safe than sorry.
Elliott says, “If symptoms ever progress beyond the skin, such as difficulty breathing, swelling, feeling faint, or vomiting, that is a serious emergency and 911 needs to be called.”
What causes hives?
Now that you’ve learned how to get rid of hives, it’s time to get to the root of the problem. The American College of Allergy, Asthma, and Immunology estimates some 20 percent of the population will deal with urticaria at some point in their lives. The main cause for all those hives typically comes down to just three things: food, medication, or illness.
Sickness
While most people think of hives as a reaction to an allergen, sometimes they’re just the body’s way of reacting to the flu or another sickness. “It’s the immune system getting funky and going awry, and the allergy system goes along for the ride,” Elliott explains.
In other words? You aren’t allergic to anything, but your body is reeling from infection. That’s why if you show up at your physician’s office with hives, doctors will typically ask if you’ve just gotten over an illness or opt to run tests for flu, strep throat, and the like.

Allergies
If you haven’t been sick and don’t sense you’re coming down with an illness, an allergy is another likely cause. While your body can react to other allergens, typically airborne environmental allergens don’t cause hives, Elliott says. “You’d really have to be rolling in it [for that to happen],” she says.
Instead, most environmental allergies cause contact dermatitis with a rash that doesn’t blanch and tends to spread. With true hives, on the other hand, typically you’re dealing with something ingested or something already going on internally, she notes.
In cases of ingested allergens, the allergy cells in your body get aggravated and then release a chemical called histamine, which causes swelling, itching, and redness. The reaction typically kicks in within 15 minutes, Elliott says, but doctors advise you to look to medicines or food you ingested within the past six hours, as there can be a delayed response.
Medication
If you’re having trouble identifying the root cause of your hives, look for patterns. Sometimes, medication can cause hives if you have an allergic reaction. Have you taken a new medicine that you’ve never taken before?
If your hives are acute—which is the case for most people who experience hives—they will go away within 24 hours, and it’s unlikely you will need to see your physician. They may come back again when you eat that one food item or take that one medication, but they’ll likely disappear once again within 24 hours, provided you don’t have contact with that allergen again.
Certain foods
Food allergies are another common cause of hives. Did you eat a new food recently? Have you had itchy welts after eating one specific food? If it happens more than once, start writing things down. If you do end up scheduling an appointment to see a physician, you’ll want to take a food diary with you when you visit the doctor.
Sometimes your allergist may recommend a low histamine diet as well, Elliott says, as histamine is contained in a variety of foods and is a common allergen.
“Ever get an itchy mouth from eating pineapple? That’s because it’s high in histamine content!” she notes. “Other foods to avoid [include] alcohol, aged cheese, processed meats, and dried fruit.”

Chronic hives
Other people have what are called chronic hives, meaning they stick around for at least six weeks. But you don’t have to wait that long to get some help: It’s when the hives just won’t go away after a week or two that the medical community recommends you visit an allergist.
During your appointment, they’ll run blood tests and sometimes targeted food allergen tests (if you notice, for example, that the hives have occurred after eating a specific food) to see if they can pinpoint the problem.
Typically adults can account for their eating habits better than kids, Elliott says, so it’s rare for doctors to have to run extensive food allergy testing on grown-ups. While you’re there, the doctor will also look for other issues going on in the body.

Autoimmune disease or cancer
On rare occasions, hives can be a signal that you’re fighting an autoimmune disease or even a blood cancer, but that tends to come with additional symptoms.
Again, Elliott is quick to point out that this is rare, but if you’ve got joint pain along with the hives, for example, or extreme fatigue, your doctor may start digging deeper to determine whether the hives are part of a larger problem or if they exist on their own.
Extreme temperatures
Some people may also suffer from hives that can be traced back to temperature triggers, says allergist Ashok Gandhi, MD, of the Marion Area Physician Group in Marion, Ohio.
For some folks, that means they experience hives in the winter when their body gets especially cold. For others, they may have a hive flare-up in sunlight.

Idopathic (unexplained) hives
But the majority of chronic hives sufferers are in Hilary H.’s boat. The hives sufferer tells HealthyWay she has lived for years with what’s known as “idiopathic hives,” meaning doctors can’t figure out why the itchy red welts crop up on her body.
“They began appearing about four years ago, and after a few months of having me try a combination of steroids and antihistamines to keep them under control, my immunologist declared them chronic,” Hilary tells HealthyWay. “When the immunology resident delivered the news that they were chronic, she prescribed antihistamines and told me, ‘You will be taking these for the rest of your existence.’”
Chronic hives remain a mystery for doctors, even the experts in the allergy field. “In a lot of chronic cases, even after all the testing, we still cannot find the reasons for hives,” Gandhi explains. Despite not knowing the cause, doctors can still help figure out how to get rid of hives.
It’s frustrating for patients, but Elliott likes to tell her patients that hives are similar to conditions such as high blood pressure in that regard. She says most people simply accept that there are many factors that could be causing their high blood pressure…and the same goes for hives. It doesn’t mean they can’t be treated, nor does it mean you can’t live a normal life. It just means you don’t know why you have the condition.
Half of chronic idiopathic (unexplained) hives cases will go away within a year, Elliott adds. If you can’t figure out how to get rid of hives, though, a visit to the doctor can’t hurt.

How to Get Rid of Hives: Takeaways
If you can determine the trigger for your hives, you’re in luck. A specific food or medication can be avoided, which means you can avoid future flare-ups.
All that said, sometimes hives show up only once, never to return again. Unless you’re seeing them repeatedly, the experts say you can often keep on living life the way you always have without fear of a recurrence. Now you know how to get rid of hives in case a flare-up pops up again.


